One in Four Have Unusual Lungs—And That May Raise Lung Disease Risk
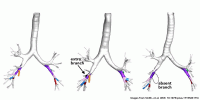
The internal anatomy of our lungs is surprisingly variable, and some of those variations are associated with a greater risk of chronic obstructive pulmonary disease (COPD), a new study from Columbia University Irving Medical Center researchers has found.
The variations occur in large airway branches in the lower lobes of the lungs and are readily detected with standard CT scans. Scans could be used to find people who are more likely to develop COPD, and the findings suggest that people with certain variations might, in the future, need more personalized treatments.
Extra and missing branches
The researchers looked at lung structure to search for COPD risk factors other than smoking.
COPD is a progressive lung disease that causes airway inflammation, makes breathing more difficult, and is the fourth leading cause of death in the United States and the world. COPD usually occurs in persons with a history of smoking, commonly after they have quit smoking, but is increasingly recognized in those who have never smoked.
“The lung’s airways function, in part, to help filter out harmful particles from the air, and airway structure affects how those particles are deposited in the lung, so we thought structure could play a role,” says R. Graham Barr, MD, DrPH, chief of general medicine at CUIMC and the study’s senior author.
“My colleague, Benjamin Smith [the study’s first author], noticed that variations in the large airways had been reported in old autopsy studies. We wanted to see how common they are in the general population and if they were associated with COPD.”
In the study, researchers examined CT scans from more than 3,000 people in the Multi-Ethnic Study of Atherosclerosis (MESA) Lung Study and found that 26 percent possessed airways that branch in a pattern that doesn’t follow the textbook model.
“The amount of lung variation high up in the airway tree was quite a surprise to us,” says Dr. Barr. “These changes are occurring at a branching level equivalent to your fingers–so it’s like a quarter of us having four or six fingers instead of five.”
About 16 percent of people possess an extra airway branch in the lung, about 6 percent are missing a branch, and another 4 percent have a combination of variants or other patterns.
People with an extra airway branch were 40 percent more likely to have COPD than people with standard anatomy. And people missing a specific airway branch were almost twice as likely to have COPD, but only if they smoked. The findings were replicated in a second study of almost 3,000 patients with and without COPD.
Paradigm of COPD is changing
About 10 percent of Americans over age 45 are believed to have COPD, which is now the nation’s fourth-leading cause of death, behind heart disease, cancer, and accidents.
Until a few years ago, relatively few researchers were looking for COPD risk factors because most believed it is almost always caused by smoking.
“Cigarette smoking is very important, and smoking avoidance and cessation is of foremost importance to reduce risk not just of COPD but also heart disease, lung cancer, stroke, and many other diseases," says Dr. Barr. "But it’s not the whole story for COPD risk.” Not all smokers get COPD, and up to 25 percent of people with COPD have never smoked. “In addition, COPD is not declining as fast as expected given the decline in smoking over the past decades.”
Newer studies of COPD show that perhaps half of people with COPD may start with low lung function early in life and the condition progresses more slowly than the classic COPD patient who smoked, says Dr. Smith, assistant professor of clinical medicine. “These people may have a different prognosis and need different treatment, and the branching patterns we found may serve as a way to identify these people and personalize risk and treatment in the future.”
Airway variants are markers of deeper anatomical changes

Drs. Barr and Smith believe that alternative central branching patterns are linked to COPD because they are indicative of deeper anatomical changes in the lung.
Advanced MRI imaging published in the study revealed that persons with an extra airway branch also had a greater number of smaller branches deeper in the lungs. Because smoke and pollution particles are captured at branch points, these lungs may be susceptible to COPD because they collect more particles.
In lungs with a missing airway branch, COPD may arise from narrower airways that occur deeper in these lungs. Narrow airways indicate that it’s harder to move air through these lungs, which may lead to more inflammation and injury in the lung.
Genetic basis for airway variants
Though the researchers need to confirm that the branching variations they reported are stable throughout life, “We think you’re born with these variations,” Dr. Barr says. When Drs. Barr and Smith looked at some participants’ CT scans from 10 years prior, the identical branching patterns were apparent.
The researchers also saw that the unusual branching patterns run in families and are probably genetically determined. They found that one variant is associated with a gene that’s known to regulate lung branching in utero and may also act to increase inflammation in more mature lungs.
Studies to address these questions are now underway.
About the study
The study, titled “Human Airway Branch Variation and Chronic Obstructive Pulmonary Disease,” was published Jan. 16 ahead of print in Proceedings of the National Academy of Sciences.
Other authors: Hussein Traboulsi (McGill Univ.), John H.M. Austin (Columbia), Ani Manichaikul (Univ. of Virginia), Eric A. Hoffman (Univ. of Iowa), Eugene R. Bleecker (Univ. of Arizona), Wellington V. Cardoso (Columbia), Christopher Cooper (UCLA), David J. Couper (UNC-Chapel Hill), Stephen M. Dashnaw (Columbia), Jia Guo (Columbia), MeiLan K. Han (Univ. of Michigan), Nadia N. Hansel (Johns Hopkins), Emlyn W. Hughes (Columbia), David R. Jacobs Jr. (Univ. of Minnesota), Richard E. Kanner (Univ. of Utah), Joel D. Kaufman (Univ. of Washington), Eric Kleerup (UCLA), Ching-Long Lin (Univ. of Iowa), Kiang Liu (Northwestern), Christian M. Lo Cascio (Columbia), Fernando J. Martinez (Cornell Univ.), Jennifer N. Nguyen (Univ. of Virginia), Martin R. Prince (Cornell Univ.), Stephen Rennard (Univ. of Nebraska), Stephen S. Rich (Univ. of Virginia), Leora Simon (McGill Univ.), Yanping Sun (Columbia), Karol E. Watson (UCLA), Prescott G. Woodruff (UCSF), and Carolyn J. Baglole (McGill Univ.).
Financial support was provided by the National Institutes of Health (R01HL130506, R01HL077612, R01HL093081, R01HL112986, RC1HL100543, RD831697, N01HC95159, N01HC95160, N01HC95169, N01HC95162, N01HC95164, U01HL114494, N01HC95159-HC95169), McGill University Health Center Research Institute, and the Fonds de la recherche en santé Québec (Quebec Health Research Fund).
One co-author (EAH) is co-founder and shareholder in Vida Diagnostics, which was used to assess some, but not the main, lung measures in the study.